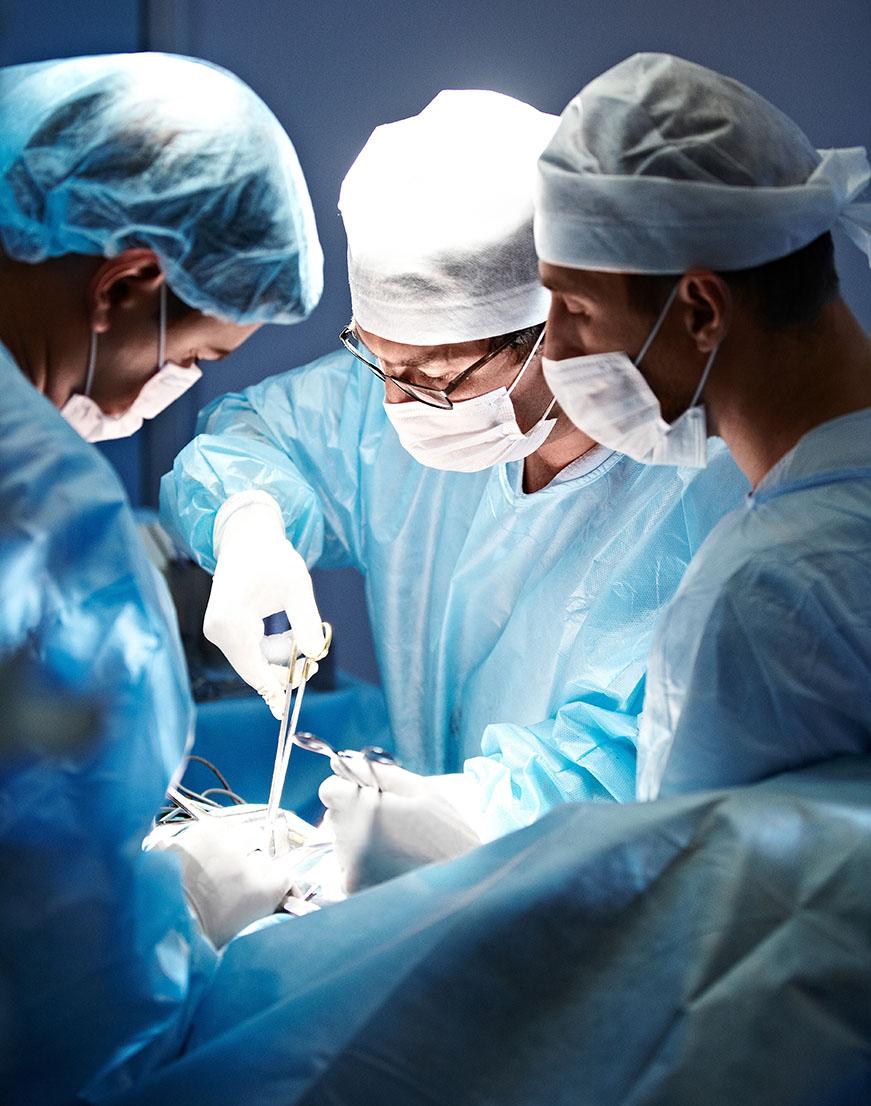
Our skilled team of surgeons specialize in general surgery, carotid artery surgery, thoracic surgery, and hernia surgery. They treat many conditions, including gastroesophageal reflux disease (GERD) and other esophageal diseases, fistulas, and gallbladder disease.
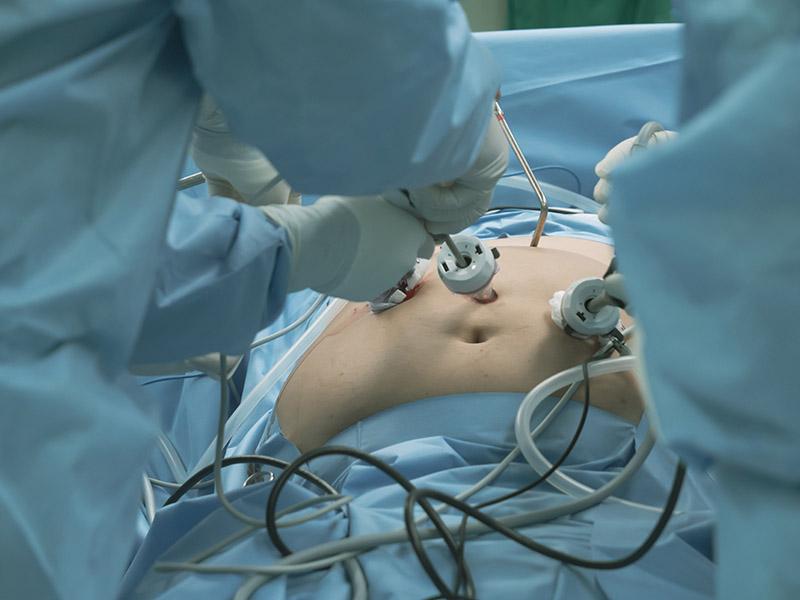
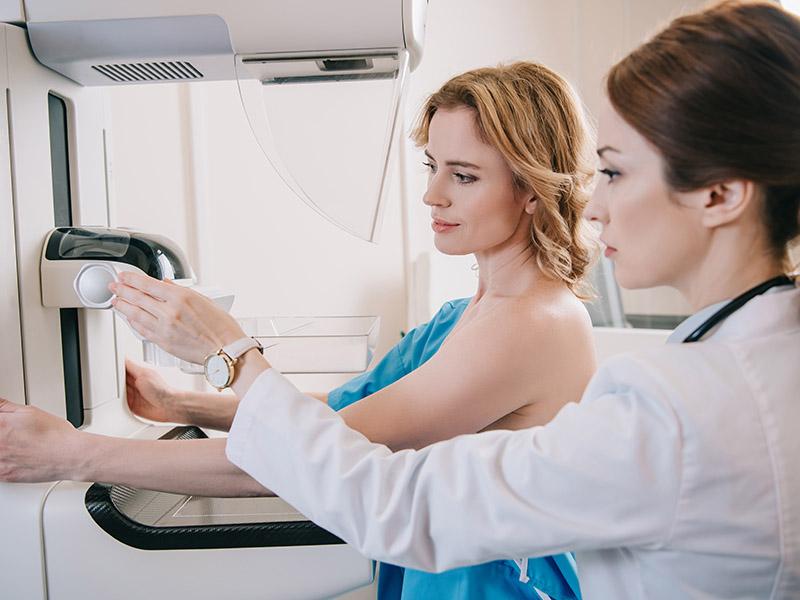
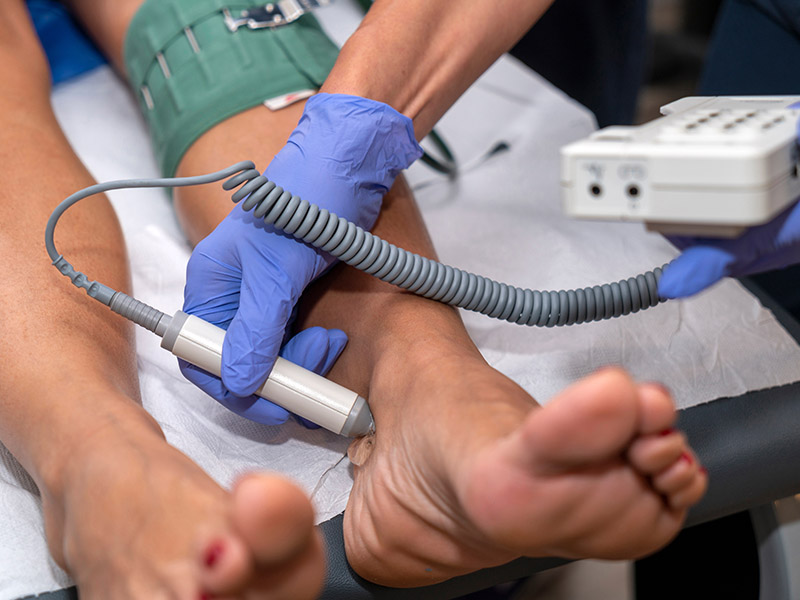
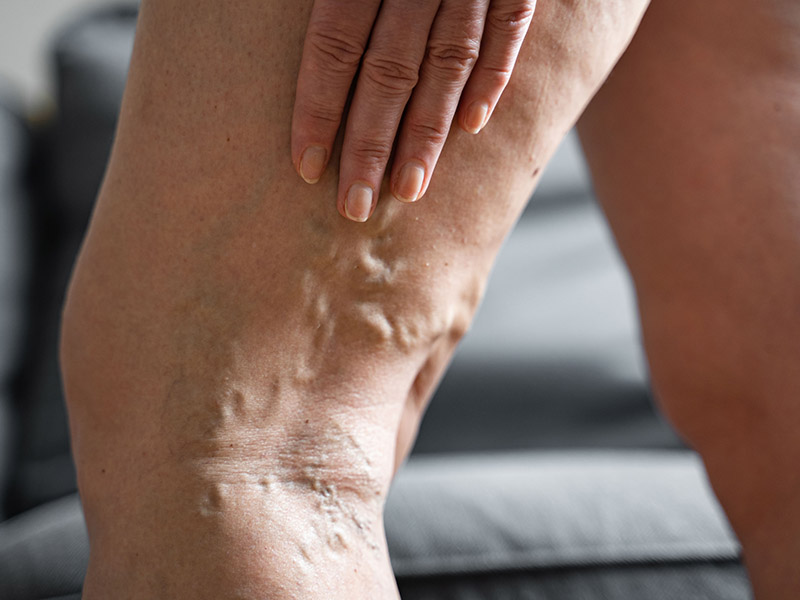
Surgical services are available to treat the underlying causes of leg pain and peripheral artery disease (PAD). The team also offers minimally invasive sclerotherapy to treat vascular insufficiency, the cause of spider veins and varicose veins. Mission Surgical Clinic offers compassionate surgical oncology services to those who need to be treated for esophageal cancer, breast cancer, and other cancers. The surgical team also provides comprehensive weight loss surgery to support healthy weight loss. Losing weight reduces your risk of developing chronic conditions like arthritis, cardiovascular disease, and other health problems linked to obesity.
The state-of-the-art surgical facilities feature up-to-date surgical technologies in a comfortable environment. The Mission Surgical Clinic team provides the highest quality patient care during surgery. They work closely with patients after surgery to ensure a healthy and safe recovery.